DRC: Thousands seek safety in hospital as fighting intensifies in North Kivu
Medical facilities supported by teams from the international medical organisation Doctors Without Borders (MSF) have received huge influxes of war-wounded patients as thousands of people flee the latest waves of armed clashes in North Kivu province in the eastern Democratic Republic of Congo (DRC). With civilians and medical facilities caught in the crossfire, MSF urgently calls on all parties to the conflict to ensure the safety of patients, medical staff and health facilities, the protection of civilians, and unhindered access for humanitarian organisations.
In the weeks following 22 January, following an escalation in armed clashes between various armed groups in the area, some 10,000 people fled their homes in and around Mweso, in Masisi territory, and sought refuge in Mweso General Hospital.
In January, and notably in the past two weeks, MSF teams in the Ministry of Health-run hospital have treated around 67 war-wounded people, mostly for gunshot wounds and injuries from explosions. More than 50 of these patients were civilians, including 21 children under the age of 15. Additionally, MSF teams have provided displaced people with psychological support and distributed temporary shelters, water filters and soap.
With fighting intensifying in Mweso over recent days, the number of people sheltering in the hospital has reduced, with many people fleeing the area towards Kitshanga, Katsiru, Nyanzale, Pinga, Kalembe and Kashunga. However, at least 2,500 people, including children whose parents have been killed, continue to shelter in Mweso Hospital.
“The situation is extremely concerning,” says MSF project coordinator Çaglar Tahiroglu. “The hospital is overwhelmed, with thousands of people crowded inside, trying to find some protection from the fighting. Alongside the Ministry of Health, we are doing our best to help everyone, but we do not have enough necessities, such as food.”
.jpg)
CONFLICT SPILLS OVER TO THE SOUTH KIVU PROVINCE OF THE DEMOCRATIC REPUBLIC OF CONGO.
Across the border in South Kivu province, where almost 155,000 people have been displaced since December 2022, according to the UN, the recent clashes have caused a new wave of displacement, with several thousand panicked people arriving in recent days in the border town of Bweremana and Minova, further south.
At the MSF-supported Minova General Hospital, medical staff treated around 30 injured people between 2 and 6 February, including four children, 10 women and 12 people requiring surgery.
With the road between North Kivu’s capital, Goma, and the town of Shasha, 27 km to the west, currently impassable due to the fighting, people are being referred from health centres in the southern part of North Kivu to Minova General Hospital and other health facilities in South Kivu, overwhelming them with patients, including rising numbers of survivors of sexual violence.
“Today, health facilities in Minova are overwhelmed and are facing shortages of essential medicines to treat common conditions such as malaria, diarrhoeal diseases, malnutrition and respiratory infections,” says Rabia Ben Alí, MSF emergency coordinator in South Kivu. “Over the past four weeks, we have seen the number of weekly cases of sexual violence treated at the hospital in Minova doubling.”
%20(1).jpg)
CAUGHT IN THE CROSSFIRE IN THE NORTH KIVU PROVINCE OF THE DEMOCRATIC REPUBLIC OF CONGO
As fighting intensifies and approaches the cities of Mweso and Minova, the safety of civilians, medical staff and patients is in increasing jeopardy.
In Mweso city centre, several houses have been hit by explosives, killing civilians. In the week of 22 January alone, an estimated 20 civilians were killed, including one child, and a further 41 were injured. In the last week of January, bullets from crossfire hit the MSF base and Mweso hospital, injuring one caregiver, while on 2 February, the area between Mweso hospital and the MSF base was hit by an explosive.
Concerned for its teams' safety, MSF has temporarily relocated some staff from Mweso and Minova.
"We continue to provide support, mostly remote, to Mweso hospital, as well as to nine health centres in the area,” says Tahiroglu. “MSF staff will return as soon as the security situation allows. However, we cannot provide medical care under these conditions, where healthcare facilities are not protected and medical staff are caught in the crossfire.”
.jpg)
VIOLENCE IN THE DEMOCRATIC REPUBLIC OF CONGO
Since March 2022, the upsurge in armed clashes in North Kivu province, linked to the resurgence of the M23 movement, has forced more than one million people from their homes and caused a humanitarian disaster in the North Kivu province, already devastated by more than 30 years of armed conflict and mass displacement.
In the Mweso health zone in Masisi territory, North Kivu province, MSF teams have been providing medical care and humanitarian aid to people affected by the violence, including some 30,000 people temporarily displaced in February 2023. In the Masisi health zone, MSF teams continue to support Masisi General Hospital and five health centres despite the difficulty of bringing in supplies with roads cut off due to the fighting. In South Kivu province, MSF teams in Minova responded to the consequences of the conflict in North Kivu during the first half of 2023. Following a deterioration in the situation, MSF launched a new emergency response in December 2023 in nine sites where displaced people had settled.
Learn more about our activities in DRC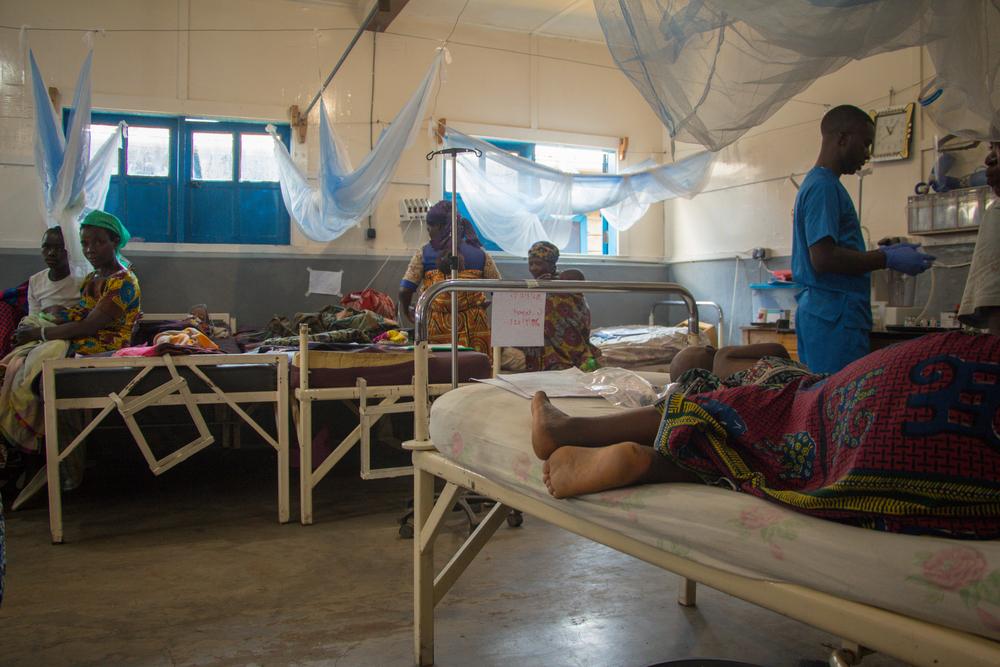
About Doctors Without Borders (MSF)
Doctors Without Borders (MSF) is a global network of principled medical and other professionals who specialise in medical humanitarian work, driven by our common humanity and guided by medical ethics. We strive to bring emergency medical care to people caught in conflicts, crises, and disasters in more than 70 countries worldwide.
In South Africa, the organisation is recognised as one of the pioneers of providing Antiretroviral Treatment (ART) in the public sector and started the first HIV programmes in South Africa in 1999. Until today, the focus of MSF’s interventions in the country has primarily been on developing new testing and treatment strategies for HIV/AIDS and TB in Eshowe (Kwa-Zulu Natal) and Khayelitsha (Western Cape).
In Tshwane, we run a migration project, and we offer medical and psychosocial care to migrants, refugees, and asylum seekers, who struggle to access public health services under South Africa’s increasingly restrictive.
Previously we offered free, high-quality, confidential medical care to survivors of SGBV in Rustenburg.
To learn more about our work in South Africa, please visit this page on our website (www.msf.org.za). To support MSF’s work:
- SMS “JOIN” to 42110 to donate R30 Once-off
- Visit https://www.msf.org.za/donate


